Are You Experiencing Symptoms of PCOS?
Do you have irregular or missed periods?
Are you experiencing unexplained weight gain or difficulty losing weight?
Have you noticed excessive hair growth on your face or body?
Are you struggling with acne or oily skin?
Do you have difficulty getting pregnant?
If any of these questions sound familiar, you might be dealing with Polycystic Ovary Syndrome (PCOS). Dr. Bernd C. Schmid specializes in diagnosing and managing PCOS, providing personalized care to help you manage your symptoms and improve your quality of life. Polycystic Ovary Syndrome (PCOS) is a hormonal disorder common among women of reproductive age, characterized by irregular menstrual periods, excessive androgen levels, and polycystic ovaries.
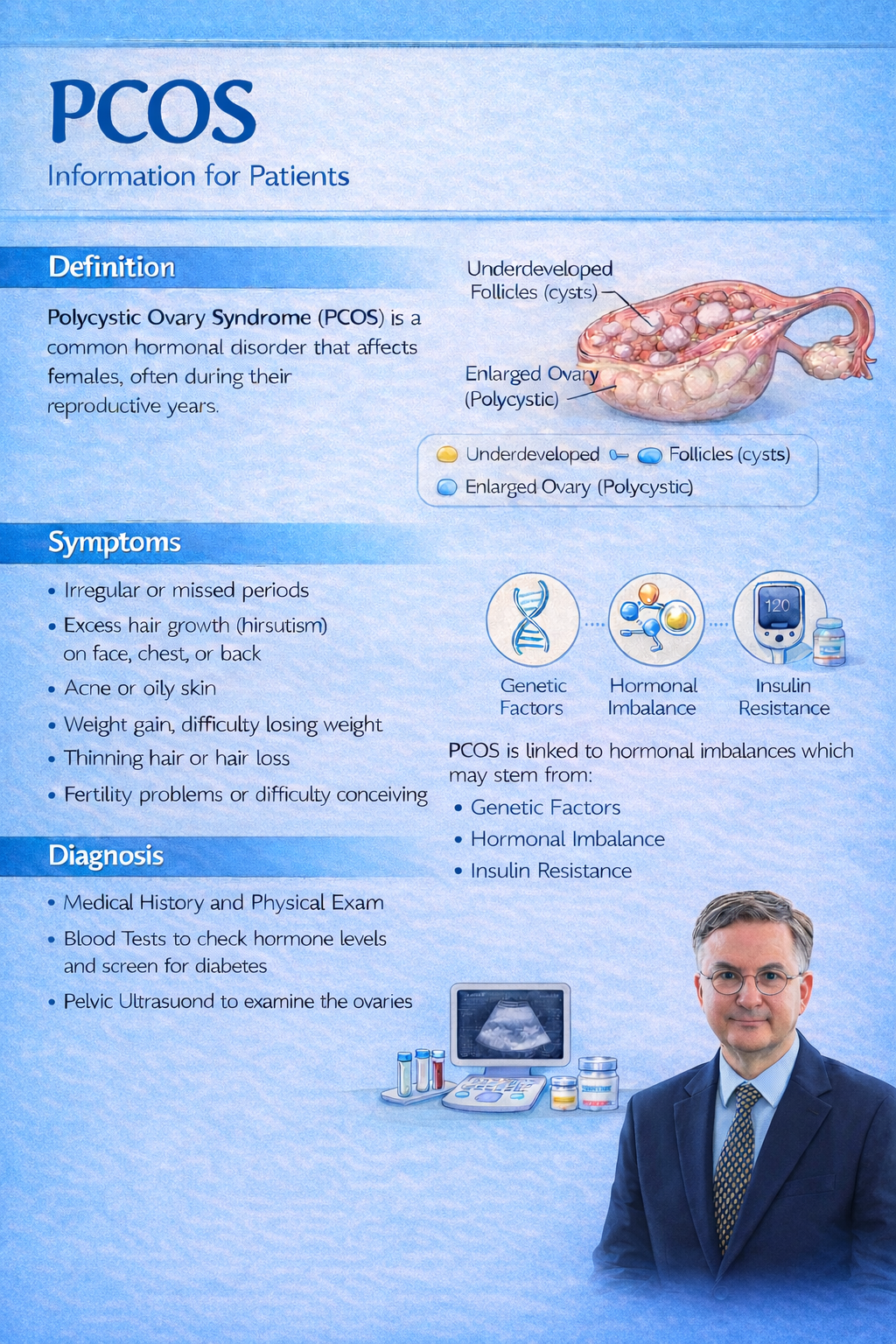
Understanding PCOS: What the evidence tells us
PCOS affects between 5 and 10 percent of women of reproductive age, making it one of the most common hormonal conditions seen in gynaecological practice. Despite this, the path to diagnosis is often frustratingly long. A large international study of over 1,300 women found that nearly half saw three or more doctors before receiving a diagnosis, and for one in three it took more than two years — with only 16 percent satisfied with the information they received along the way (Gibson-Helm et al., Journal of Clinical Endocrinology & Metabolism, 2017). At Dr. Schmid's practice in Robina, Gold Coast, a thorough and timely approach to diagnosis is a priority from your very first appointment.
What causes PCOS symptoms?
The core problem in PCOS is a hormonal imbalance that drives higher-than-normal androgen (male hormone) levels, disrupted ovulation, and often — though not always — changes in how the body handles insulin. These shifts explain the wide range of symptoms women experience: irregular or absent periods, acne, excess facial or body hair, scalp hair thinning, difficulty conceiving, and weight changes. Not every woman will have all of these features, which is a key reason the condition is so often missed.
How is PCOS diagnosed?
Diagnosis uses the Rotterdam criteria, which require two out of three of the following: irregular ovulation, signs of elevated androgens, and a characteristic ovarian appearance on ultrasound. Polycystic-looking ovaries alone are not enough — the full clinical picture matters. Blood tests help rule out other conditions with similar presentations, including thyroid disease and elevated prolactin levels.
Treatment: What the evidence supports
Treatment is tailored to what matters most to you right now.
If you are not currently trying to conceive, the main goals are regulating your cycle, managing symptoms such as acne and unwanted hair growth, and protecting the uterine lining. Current international guidelines — including the 2023 international evidence-based PCOS guideline (Teede et al., European Journal of Endocrinology, 2023) — support combined oral contraceptives as first-line pharmacological therapy for menstrual regulation and androgen excess. Where hair growth remains troublesome after several months, an antiandrogen medication such as spironolactone may be added. Lifestyle changes, particularly modest weight loss of 5 to 10 percent of body weight, have been shown to restore ovulatory cycles and improve metabolic markers in multiple studies, independent of medication.
If you are trying to conceive, ovulation induction is the focus. A landmark randomised trial published in the New England Journal of Medicine (Legro et al., 2014) — the largest of its kind at the time — demonstrated that letrozole produced significantly higher live birth rates than clomiphene citrate in women with PCOS, particularly those with higher BMI. Letrozole is now the preferred first-line agent. For women who do not respond to oral medications, laparoscopic ovarian drilling — a minimally invasive keyhole procedure — is an established surgical alternative. A Cochrane review confirmed that ovarian drilling produces comparable pregnancy rates to gonadotropin injections with a lower risk of multiple pregnancy and ovarian hyperstimulation syndrome (Farquhar et al., Cochrane Database of Systematic Reviews, 2012). Dr. Schmid performs this procedure at Gold Coast Private Hospital.
For women with PCOS and significant obesity where other treatments have not been successful, bariatric surgery is increasingly recognised as a meaningful option. The BAMBINI trial — a multicentre randomised controlled trial published in The Lancet (Samarasinghe et al., 2024) — found that women with PCOS and BMI over 35 who underwent laparoscopic sleeve gastrectomy were nearly 2.5 times more likely to resume spontaneous ovulation at 52 weeks compared with those receiving medical therapy alone.
Metabolic health matters long-term
Women with PCOS face a higher lifetime risk of type 2 diabetes and cardiovascular disease. An oral glucose tolerance test at diagnosis, along with lipid and blood pressure monitoring, is recommended by international guidelines and forms part of the initial assessment at this practice.
Mental health and PCOS
Research consistently shows that women with PCOS experience higher rates of depression and anxiety. A cross-sectional study also found that women with PCOS reported less trust in their treating doctors and greater dissatisfaction with their care compared with women without PCOS (Lin et al., Journal of the Endocrine Society, 2018) — a finding that underlines why clear communication and a thorough explanation of your diagnosis matters.
Dr. Schmid's approach
Dr. Schmid offers a comprehensive initial consultation covering diagnosis, metabolic risk assessment, and a personalised management plan — whether your priority is symptom control, fertility, or long-term health. His surgical experience includes laparoscopic procedures for both gynaecological and fertility indications, performed at Gold Coast Private Hospital, Robina.
Clinical content on this page draws on current international evidence, including guidelines from Teede et al. (2023), and landmark trials published in the New England Journal of Medicine, The Lancet, and the Cochrane Database of Systematic Reviews.
